Understanding High-Smile Lines
A high-smile line means more of the gums show above the upper front teeth when you smile. It is a normal variation, but it can draw attention to the gums rather than the teeth. Understanding what causes it helps plan safe, conservative changes if reduction is considered. Clear terms and measurements guide good decisions.
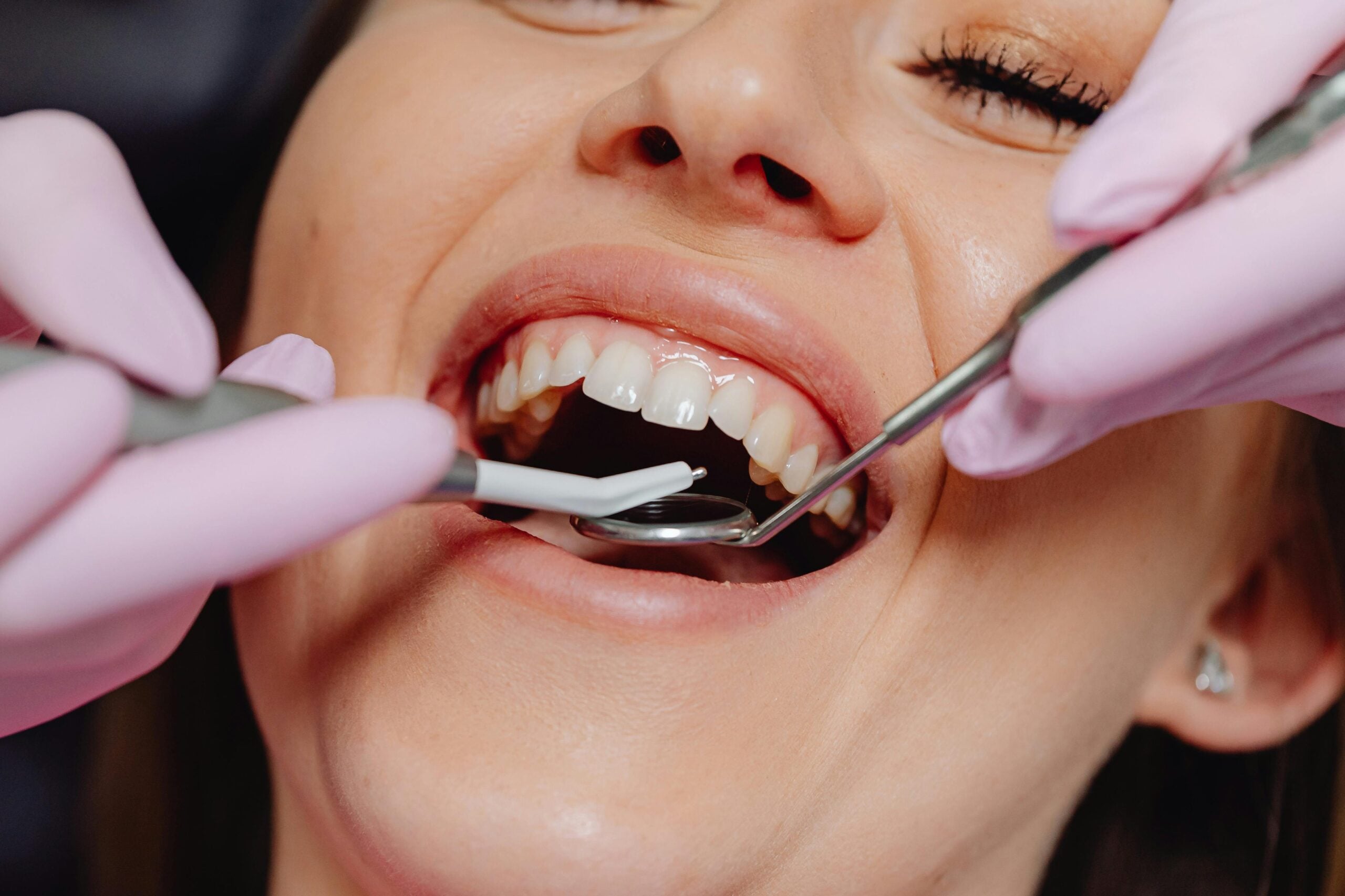
Someone laughs and shows several millimeters of gum above the teeth. A high-smile line often results from a mix of factors: short or hypermobile upper lip, short clinical crowns, delayed or altered passive eruption of teeth, vertical maxillary excess, or dentoalveolar extrusion. Each factor changes how much tooth and gum appear during a full smile. Because causes differ, the approach to reducing gum display must be tailored.
Assessment starts with photos and measurements at rest, social smile, and full smile. We note upper incisor display in millimeters, lip mobility, and gingival display. Bone levels and the cemento-enamel junction are evaluated with gentle probing and radiographs to see if gingival reshaping will keep a healthy biologic width. These steps ensure function and gum health are protected before any reduction is planned.
- Measure incisor display at rest and full smile
- Record lip length and mobility
- Map gingival margins, papillae, and smile arc
- Evaluate crown length relative to bone and CEJ
- Screen for vertical maxillary excess and dental extrusion
- Review periodontal health and keratinized tissue
When causes are identified, options can be combined thoughtfully. Gingival recontouring may help when gum margins sit too far coronally, while orthodontic intrusion addresses dental extrusion. Skeletal issues sometimes need surgical consultation. After tissue or tooth position changes, careful restorative shaping may refine the smile line, for example with precision-made crowns and bridges when teeth need new contours and support. This overview supports high smile reduction guide planning for predictable, patient-centered results.
If you are considering changes, a clear diagnosis and simple measurements make choices safer and more effective.
Importance of Alveolar Reduction Planning
Alveolar reduction planning matters because bone position controls where the gums can heal and stay stable. When extra gum shows in a high smile, careful planning sets safe targets for bone reshaping so gumlines match the desired tooth display. Good plans protect roots and papillae, keep the bite comfortable, and reduce the chance of relapse.
Picture a full laugh where gums show more than you want. If only soft tissue is trimmed but the bone is left too close to the tooth, the gums often rebound to their old height, or become inflamed. Planning alveolar reduction creates healthy space for the gum attachment, which supports lasting crown length and comfortable brushing. It also lets the dentist match tooth height-to-width and the smile arc without harming support around neighboring teeth. This alignment of biology and esthetics is the core reason planning comes first.
Planning starts by mapping each tooth’s cementoenamel junction, current gum level, and the crest of the bone using probing and targeted radiographs. The thickness and shape of the bone are reviewed so the sculpting follows the natural scallop, while preserving the peaks between teeth that keep papillae full. The plan is sequenced with tooth position, since intrusion or alignment may reduce how much bone reshaping is needed; in some cases, limited clear aligner care such as Invisalign can be coordinated before gum surgery. Surgical access, incision design, and suturing are then chosen to protect keratinized tissue and speed healing. These steps also help set realistic healing timelines before final restorations.
Planning links surgery to the final look and function. It clarifies when to finish with conservative bonding or when new contours with porcelain veneers will best frame the new gumline. It also anticipates sensitivity, root exposure risks, and cleaning needs, so home care remains simple. Thoughtful alveolar reduction is central to high smile reduction guide planning and long-term stability. A measured plan leads to healthier, steadier results.
Utilizing High-Smile Photos in Treatment
High-smile photos show your widest, most natural smile, which is when extra gum is most visible. We use these images to measure tooth display, gum display, and lip movement in millimeters. The photos guide safe choices for soft tissue, bone, and tooth changes, and help set clear goals you can see. They also create a shared reference for you, the dentist, and the lab.
You laugh for the camera and show 4 mm of gum. We take photos at rest, social smile, and full smile, keeping the head level and the camera square to the face. A simple calibration step, such as a small ruler in one photo, turns pixels into millimeters, so we can compare visits and track changes. Landmarks like the incisal edges, midline, and gingival zeniths are marked, then measured to plan new margins and edge positions. Standardized smile photographs allow objective measurement of gingival display that supports treatment planning [1].
After measurements, we overlay conservative targets to test how much change is needed to meet your goals. If most display comes from short clinical crowns, photos help us estimate how much gum and bone recontouring might be required, and how that will affect tooth proportions. If the issue is tooth position, the same images show whether minor orthodontic intrusion would help before gum surgery. Photos also guide finishing steps, like edge smoothing or small shape changes with precise dental bonding, so the final smile matches the plan.
Color and brightness matter too. Reviewing high-smile photos under similar lighting helps choose a shade and decide if timing a round of professional teeth whitening before any contouring will improve the overall look. These photos then serve as a baseline to check healing and stability at each visit. They fit neatly into high smile reduction guide planning by linking measurements to realistic results. If you plan to stop by, see our current hours. Clear photos make safer, steadier decisions.
Assessing A-P Spread for AOX
Assessing A-P spread for AOX means measuring how far the planned implants span from front to back in a full-arch restoration. This measurement sets safe limits for any back-end cantilever and where the teeth can sit. It helps protect implants from overload and supports a stable, comfortable bridge. We confirm it on scans and digital models before surgery.
You want a stable full-arch bridge that does not flex when you chew. We assess A-P spread by first setting the target incisor edges from photos, speech sounds, and facial support. Then we map the back tooth positions needed for a balanced bite. On the CBCT and digital plan, we place the anterior implant and the two most posterior implants within anatomic limits. The A-P spread is the front-to-back distance from that anterior position to the line joining the posterior implants, and a broader spread allows a shorter, safer cantilever.
Several factors influence this distance. Angled posterior implants can increase spread while staying clear of the sinus or nerve, and arch shape, bone density, and implant diameter all play roles. Alveolar reduction creates restorative space and ideal crown height, which supports a rigid, cleansable framework, but it does not replace the need for adequate spread. These checks help confirm whether a fixed full-arch option such as thoughtfully planned All On 4 implant dentures is appropriate for your bite and smile.
If spread is limited, options include shortening the distal tooth run, changing implant angulation, or adding a posterior implant. In some cases, a removable pathway like well-designed snap-in implant dentures reduces cantilever demands and can simplify home care. Accurate A-P spread assessment ties esthetics to strength, fitting smoothly into high smile reduction guide planning. One clear measurement supports steady chewing and long-term comfort.
Step-by-Step Reduction Guide
This guide outlines how we safely reduce excess gum display in a high smile. We move from careful measurements to tissue shaping, then finish with refined tooth form. Each step protects gum health and tooth support while aiming for a natural look. Clear checkpoints keep decisions simple and predictable.
You smile wide and show more gum than you prefer. We begin with standardized photos at rest, social smile, and full smile, then convert pixels to millimeters for accurate targets. Probing and focused radiographs map the cemento-enamel junction and bone crest so planned margins remain biologically stable. A digital or wax preview sets desired tooth length and smile arc, letting us test small changes before any procedure. Comfort planning, including local anesthesia and, when appropriate, comfortable oral sedation options, is reviewed so the visit feels manageable.
On the day of treatment, we mark the new gingival margins using the preview as a guide. If soft tissue alone is thick or too far coronal, precise trimming can reshape levels. When bone sits close to the tooth, a small flap is gently reflected to sculpt the crest, creating healthy space for the gum attachment. The scallop is blended tooth by tooth, and papilla peaks are preserved for natural fill between teeth. The tissue is sutured to its new position, and smooth contours make cleaning straightforward during healing.
After two to three weeks, early healing is reviewed, and small edge adjustments or polishing can fine tune the result. Final proportions are confirmed once tissues stabilize, often over several more weeks, using new high-smile photos to verify symmetry and tooth display. If needed, conservative bonding or minor alignment can complete the plan without over-treating. These steps create a steady path from diagnosis to finish and fit within thoughtful high smile reduction guide planning. One careful sequence leads to healthy, lasting smile changes.
Common Challenges in High-Smile Reduction
High-smile reduction is challenging because different causes often overlap. The main hurdles are finding the true source of excess gum show, setting safe limits so gums remain healthy, and correcting asymmetry without flattening the smile. Thin gum types raise the risk of recession, and results can slip back if bone position is not considered. Clear goals and realistic timelines reduce surprises.
You smile wide and one side shows more gum than the other. Diagnosis can be tricky because short clinical crowns from altered passive eruption, dentoalveolar extrusion, a hypermobile lip, or vertical maxillary excess may look similar. Each cause points to a different solution. If the gum margin is high because the bone crest sits close to the tooth, trimming soft tissue alone often heals back toward the old level. When tooth position is the driver, minor intrusion or alignment can reduce display without aggressive tissue work. Getting that distinction right prevents overtreatment and improves stability.
Biology sets limits that are easy to miss. A thin periodontal biotype is more prone to recession, especially if new margins are placed with inadequate keratinized tissue or the bone scallop is flattened. Creating proper space for the attachment while preserving the peaks between teeth helps avoid black triangles and maintains papilla fill. Root proximity, existing restorations, and uneven CEJ locations can complicate bone reshaping and require tooth-by-tooth adjustments. Occlusion and speech also matter, since longer incisors can change bite contacts and “S” sounds if planned lengths exceed functional space.
Timing is another common challenge. Swollen tissue can hide the final margin for weeks, so finishing esthetics too early risks asymmetry later. Patients may expect instant symmetry, yet the healthiest results come from staged checks with updated high-smile photos. Comfort planning helps too, and longer procedures may be easier with thoughtful deep sedation care when appropriate. Naming these challenges early strengthens high smile reduction guide planning and supports steady, lasting results. Careful diagnosis and sequencing protect both esthetics and gum health.
Techniques for Accurate Smile Analysis
Accurate smile analysis uses standardized photos and video, calibrated measurements, and clear facial landmarks. We compare rest, social, and full smiles, then record tooth and gum display in millimeters. These records, combined with a focused exam and radiographs, show how lips, teeth, gums, and bone work together. The result is a clear map that guides safe, predictable changes.
You smile for a photo and your gums show the most. To make measurements reliable, we keep the head level, eyes forward, and the camera square to the face. A small reference, such as a millimeter ruler in one image, lets pixels convert to exact millimeters for repeatable tracking. Short video or burst photos help capture the true peak smile, which is often the key moment for planning. Phonetic checks with “F” and “S” sounds confirm where incisal edges should sit during speech.
Next, we align features to stable landmarks. The interpupillary line helps level the smile, and the facial midline centers the teeth. We mark incisal edges, gingival zeniths, and the smile arc, then review tooth width-to-length so new targets look natural and function well. Lip length and mobility are measured to see how much the lip moves from rest to full smile, since this often drives visible gum. Periodontal sounding and selected periapical radiographs show the distance from the gum margin to the bone crest, which helps set safe limits for any margin change.
Digital overlays or a small mock-up test proposed tooth lengths and gum levels before any procedure. If orthodontic alignment or light intrusion will help, we note that sequence so tissue changes are minimal and stable. All records are organized into a reference set for the lab and surgeon, which keeps contours, symmetry, and timing aligned across the team. These techniques support high smile reduction guide planning by turning photos and numbers into a stepwise, conservative plan. Clear measurements lead to safer decisions and steadier results.
Post-Planning Considerations for Success
After planning, success depends on how well tissues heal, how the bite feels, and when final work is finished. We watch for gum stability, protect the area during healing, and confirm that speech and chewing feel natural. Clear checkpoints guide when to adjust, when to wait, and when to finalize. This steady follow-up helps the result last.
Picture a two-week check where gums still look slightly puffy. Early swelling is normal, and margins can appear uneven until tissues mature. We review photos taken before treatment to compare gum levels and tooth lengths, then confirm that new margins are stable across several visits. Provisional shapes help guide the gum line and papilla fill, so we refine them first, and delay final restorations until the tissue position holds steady. This timing reduces the chance of soft-tissue rebound and improves symmetry.
Bite comfort matters as much as looks. Longer front teeth can change how top and bottom teeth touch, so we test light tapping and side movements, then make small adjustments if needed. If clenching is present, a simple night guard can protect new edges while tissues mature. For cases that included orthodontic intrusion, retainers are used as directed to prevent relapse while the bone and ligaments settle. These steps protect both the smile line and the supporting structures.
Home care should stay gentle and consistent. A soft brush and careful technique keep healing margins clean without irritation. Sensitivity can appear as exposed root surfaces adjust; it often improves as tissues thicken and habits normalize. If tooth color changes are planned, whitening is best completed and shade stabilized before new veneers or crowns are matched. Standardized high-smile photos at follow-ups verify that gum display remains even and that speech sounds like “S” and “F” are clear. This practical approach fits neatly into high smile reduction guide planning.
Finally, a maintenance schedule locks in gains. Short-term checks confirm stability and hygiene, then routine visits monitor the smile line over time. When biology, bite, and timing work together, results feel natural and stay steady. Thoughtful follow-up keeps the smile healthy and predictable.
Updates in High-Smile Line Techniques
Today’s high-smile line care focuses on precise diagnosis and smaller, better‑targeted changes. Updates include digital planning, tissue‑preserving surgical steps, and coordinated orthodontic moves that reduce excess gum show while protecting health. The aim is predictable gum levels, natural tooth proportions, and comfortable cleaning. Plans are customized to the cause, not one procedure for everyone.
A patient smiles and shows 5 mm of gum despite normal tooth length. For tooth‑related causes, biologic crown lengthening now starts with calibrated photos, periodontal sounding, and CBCT where needed, then a mock‑up to test final margins. Surgeons often use fine microsurgical instruments, papilla‑sparing designs, and piezo or micro‑burs to sculpt bone in small increments. When adequate enamel and bone spacing allow, limited soft‑tissue recontouring with careful thickness checks can help, but modern plans avoid trimming alone if bone is too close. Digital overlays and printed guides translate millimeter targets to the mouth, improving symmetry and reducing guesswork.
When the upper lip is the driver, updates favor stepwise, reversible trials before surgery. Small‑dose neuromodulator treatment can test whether reducing lip lift achieves the goal, offering a temporary preview without altering teeth or bone. If stability is confirmed, refined lip‑repositioning techniques use conservative flap design and tension control to limit relapse and maintain smile contour. For tooth position issues, light orthodontic intrusion is planned first, often with clear aligners plus intrusion attachments or temporary anchorage devices for precise millimeters of movement. Skeletal vertical maxillary excess remains a jaw problem, so coordinated orthognathic care may be the most stable choice when gum show is large. These pathways prevent over‑treating soft tissue when the foundation needs correction.
Across options, healing and timing are managed more deliberately. Provisional contours guide the gumline while tissues mature, then final contours follow once measurements hold steady over several visits. Teams share standardized high‑smile photos and simple millimeter goals so the surgeon, orthodontist, and lab stay aligned. These updates fit neatly into high smile reduction guide planning by linking diagnosis, sequence, and maintenance into one clear roadmap. One careful sequence improves stability and comfort.
Future Trends in Smile Enhancement
Smile enhancement is moving toward precision planning, smaller interventions, and results you can preview in motion before treatment. Digital records, 3D models, and measured targets guide steps so gum levels and tooth lengths stay stable. Teams combine orthodontic, surgical, and restorative care in a clearer sequence. The goal is a natural look that is easier to clean and maintain.
Imagine seeing a short video of your own future smile before any procedure. New workflows capture dynamic smiles, then merge photos, scans, and CBCT into one facially guided plan. Artificial intelligence helps measure lip movement and symmetry, which improves target setting. Printed guides and navigated surgery transfer millimeter plans to the mouth, reducing guesswork while protecting papillae and bone peaks.
Tissue care is becoming more conservative. Surgeons favor microsurgical flap design, piezo or fine burs for controlled bone sculpting, and techniques that preserve keratinized tissue. For thin gum types, soft tissue thickening with carefully selected grafts or biomaterials can improve stability and reduce recession risk. When lip hypermobility drives gum show, temporary neuromodulator trials help confirm goals, and refined lip-repositioning methods focus on tension control and contour. If tooth position is the cause, light intrusion with clear aligners or small anchorage devices delivers measured millimeters before any tissue change.
Finishing and follow-up are getting smarter too. Intraoral scanners create accurate provisionals that guide the healing gumline, and small adjustments are timed to tissue maturity. Remote photo checks and standardized high-smile images allow the team to confirm symmetry and hold final contours until measurements are steady. These tools support high smile reduction guide planning by linking diagnosis, sequence, and maintenance in one roadmap. The result is more predictable healing and a smile that feels natural.
For patients, the trend means clearer previews, fewer surprises, and simpler care at home. Careful planning, smaller steps, and steady follow-up build lasting, comfortable changes. Thoughtful planning leads to steadier smiles.
Frequently Asked Questions
Here are quick answers to common questions people have about Planning Reduction Using High-Smile Lines in Glendale, AZ.
- What causes a high-smile line?
A high-smile line can result from various factors, including a short or hypermobile upper lip, short clinical crowns, delayed or altered passive eruption of teeth, vertical maxillary excess, or dentoalveolar extrusion. Each of these factors influences how much tooth and gum are visible during a full smile. Understanding the specific cause for each individual is key to tailoring an effective treatment plan that can reduce gum display while maintaining healthy gum and tooth function.
- Why is thorough planning important before reducing a high-smile line?
Thorough planning is crucial because it ensures the stability and health of both gums and bone post-procedure. Without planning, there’s a risk the gums may heal back to their original position or become inflamed. Proper planning considers bone reshaping, protects dental roots, aligns teeth, and reduces the chance of aesthetic relapse. This comprehensive approach balances biological and aesthetic factors, ensuring long-term success and satisfaction with the smile enhancement.
- How do photos help in planning for high-smile line reduction?
Photos are essential for planning high-smile line reduction because they provide a visual guide to assess the current gum and tooth display, lip movement, and overall smile. By measuring these elements in millimeters, photos help determine the necessary adjustments for gums, bone, and teeth. They also serve as a shared reference point between the patient, dentist, and lab, ensuring everyone is aligned on the desired outcome.
- Can orthodontics help in reducing a high-smile line?
Yes, orthodontic treatment can help reduce a high-smile line, especially if dental extrusion is a contributing factor. Orthodontic intrusion, for example, can reposition the teeth vertically, minimizing excess gum display. This approach can sometimes reduce the need for more invasive procedures, such as gum or bone reshaping, by addressing the underlying cause of the high-smile line.
- What are the common challenges in reducing a high-smile line?
Common challenges include correctly diagnosing the overlap of potential causes, setting safe limits to preserve gum health, and ensuring symmetrical results. Risks such as gum recession or the gums reverting to their original position if the bone is not addressed must also be considered. These challenges require careful planning and a customized approach to each unique case to achieve a successful outcome.
- How do you ensure long-term success after high-smile line reduction?
Long-term success after high-smile line reduction depends on factors like tissue healing, maintaining a comfortable bite, and timing final restorations properly. Regular follow-ups help monitor stability and symmetry, while provisional shapes guide gum lines during healing. Effective home care and, if needed, a night guard for bite comfort are also key components in preserving the desired results over time.
References
- [1] [Measurement and analysis of smile line of 62 Han-Chinese]. (2011) — PubMed:22333304