Understanding CBCT Imaging Technology
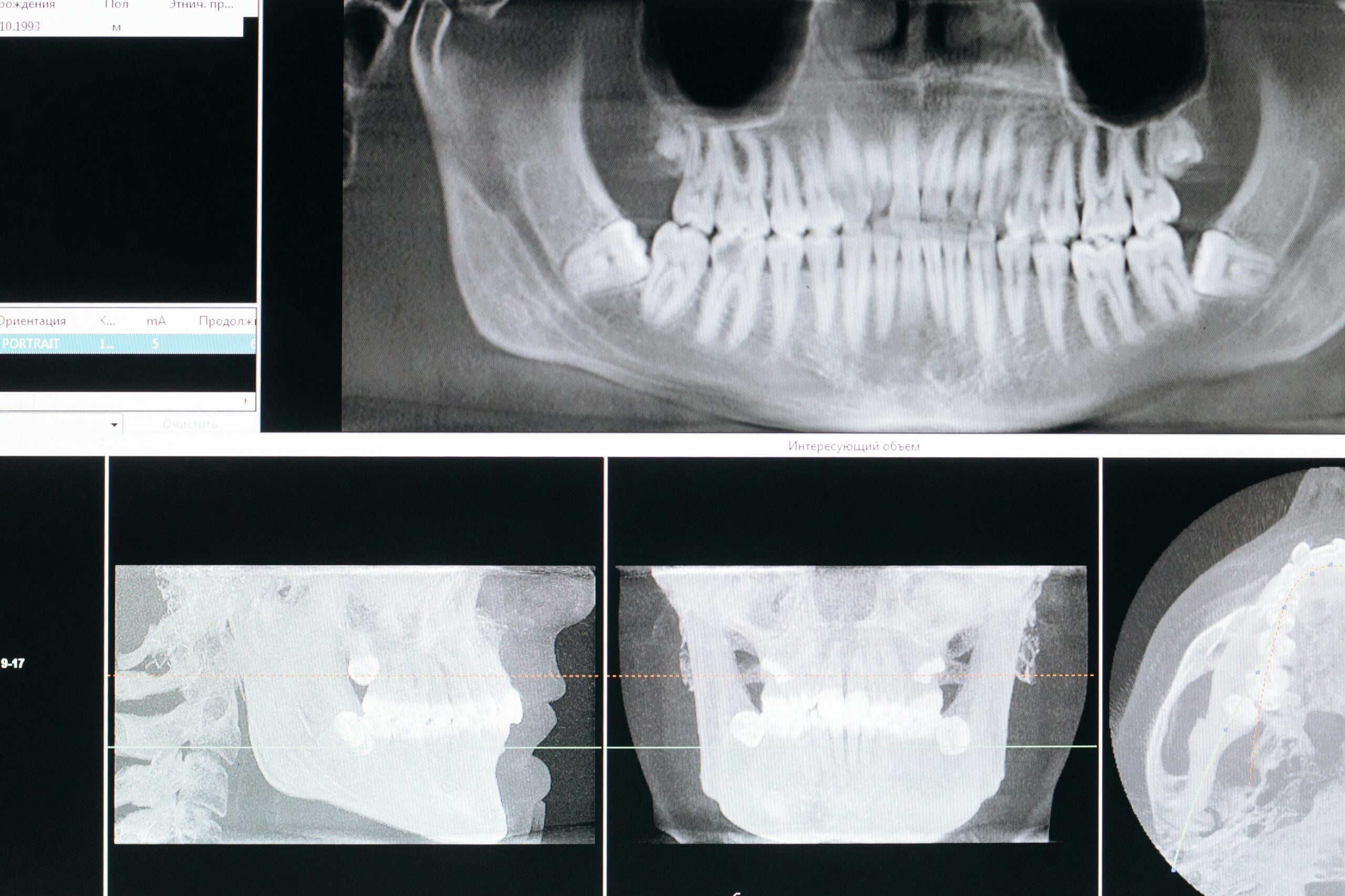
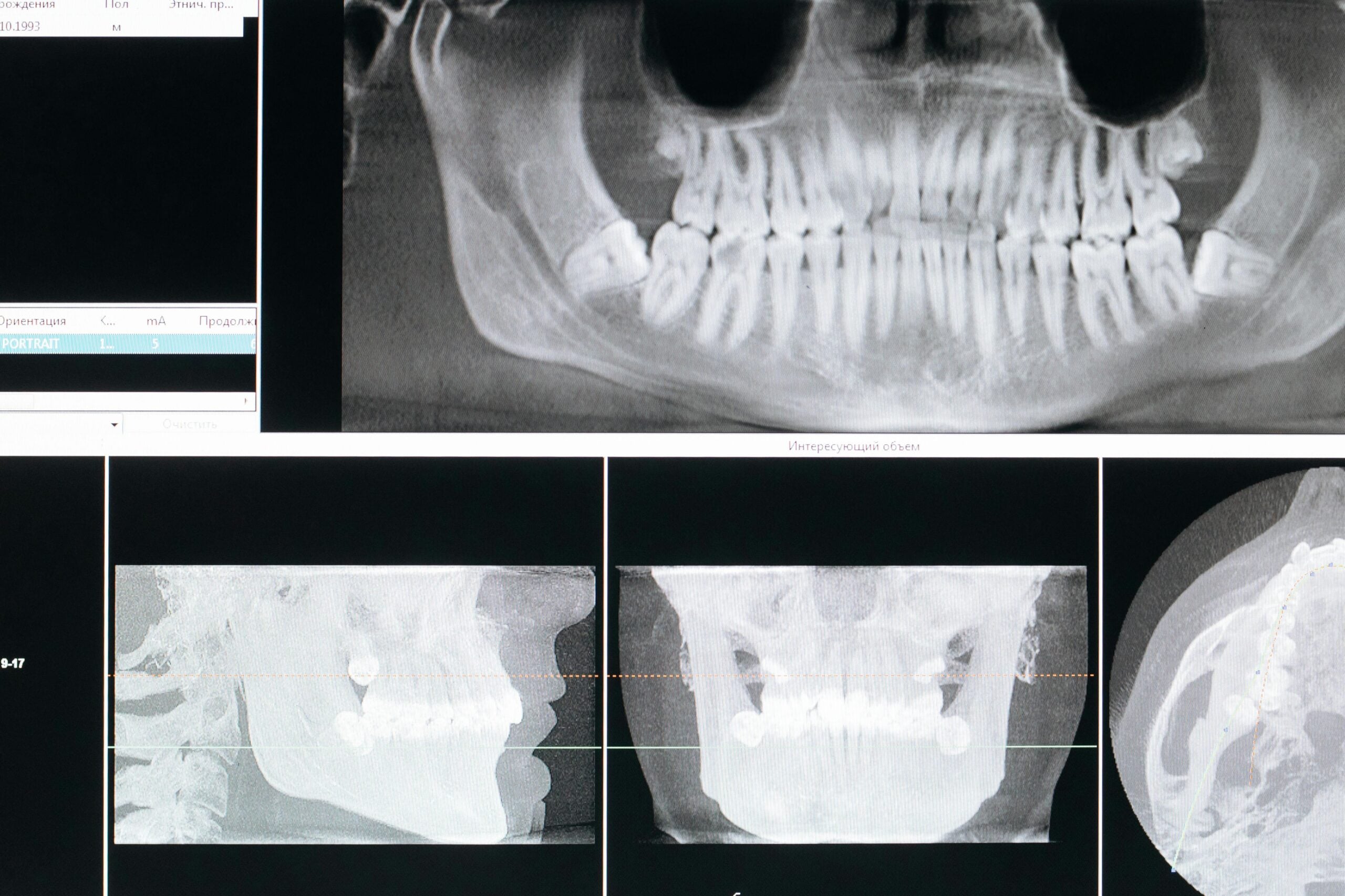
Cone beam computed tomography, or CBCT, is a 3D dental imaging system. It creates detailed views of teeth, jaws, nerves, and sinuses in a single, quick scan. Picture a 3D map of your jaw before a dental implant. Questions about cbct scan safety are common, and we address the basics here.
CBCT uses a cone-shaped x‑ray beam that rotates around your head. A detector captures many images in seconds, which software rebuilds into a 3D volume. The dentist can view thin slices from any angle, zoom in on areas of concern, and measure distances with precision. Field of view can be kept small, which helps focus on the problem area and limit exposure.
What does a CBCT show that 2D x‑rays may miss?
- Exact tooth root shapes, extra canals, and hidden fractures
- Locations of nerves, sinuses, and blood vessels to avoid
- Jawbone width, height, and density for implant planning
- Impacted teeth, cysts, or other unusual findings
Clinically, this matters when placing implants, evaluating complex infections, and planning surgeries. For example, it can guide the safest path and depth for an implant, and it helps find missed canals or cracks before retreatment. It can also clarify the position of impacted wisdom teeth or roots near the sinus. When indicated, CBCT supports careful diagnosis and fewer surprises during complex root canal treatment.
Safety is managed by using the smallest field of view that answers the question, and only scanning when it will change care. A CBCT involves more radiation than a single small dental x‑ray, but much less than a hospital medical CT of the same region. Scans are brief, typically under a minute, and you remain seated while the unit rotates. Collimation, proper settings, and evidence-based selection help keep exposure as low as reasonably achievable while still providing the detail needed for tasks like planning full arch implant dentures. Understanding how CBCT works helps you see why, and when, it may be recommended.
CBCT provides focused 3D detail to support safer, more accurate dental care.
How CBCT Scans Work
A CBCT scan uses a cone-shaped x‑ray beam and a detector that rotate once around your head. During that single turn, the system records many snapshots from different angles. A computer then rebuilds those snapshots into a 3D model of your teeth, jaws, and nearby structures. You sit still, usually for less than a minute, while the unit captures the data.
Think of each snapshot like a shadow from a new viewpoint. The software stacks these shadows using math to create tiny 3D blocks, called voxels, that form the final image. Smaller voxels can show finer detail, which is helpful for tasks like checking a thin bone wall, while larger voxels reduce file size and exposure. The x‑ray beam is pulsed, not continuous, which helps collect clear images with short bursts of radiation. Careful head positioning, bite support, and motion tracking reduce blur so measurements stay accurate.
Before scanning, the dentist selects a field size that covers only what is needed. The machine then limits the beam to that region, improves contrast for bone and teeth, and applies tools that lessen streaks from metal. The result is a 3D volume that can be sliced in any plane, measured to fractions of a millimeter, and matched to planned treatments. Short scenario: mapping a lower wisdom tooth root near a nerve. This is why CBCT is often used to plan safer wisdom tooth removal.
Understanding how the system collects and rebuilds data also explains cbct scan safety steps, such as picking the smallest scan that answers the question and scanning only when it may change care. For you, this means fewer surprises, clearer conversations about options, and images tailored to the problem at hand. In the next section, we will look at when CBCT is appropriate and how clinicians decide.
Radiation Exposure in Dental Imaging
Dental imaging uses x-rays in small, targeted amounts to answer specific clinical questions. Exposure varies by the type of exam, the size of the area scanned, and the settings chosen. For CBCT, dentists limit the beam to the smallest region that solves the problem and select protocols that balance detail with dose. These choices keep exposure low while producing images that guide safe care.
Short scenario: checking a cracked tooth root without scanning the whole jaw. Radiation is discussed as “effective dose,” which estimates overall risk by considering which tissues are exposed. In practice, dose changes with field of view, voxel size, tube current and voltage, filtration, rotation method, and patient size. Even panoramic units show measurable dose differences when rotation axis and exposure modulation are adjusted, which is why protocols matter [1]. CBCT systems also use pulsed beams and tight collimation to reduce scatter and limit exposure to nearby tissues.
Some situations need extra care. During pregnancy, dental bitewing x-rays deliver extremely low fetal doses in Monte Carlo models, far below levels associated with harm [2]. For children, clinicians justify each image carefully, choose child-sized fields, and use settings designed for smaller patients. Technology also helps. Newer reconstruction methods can produce useful low-dose CBCT images, which may reduce exposure further when detailed 3D information is needed [3]. Together, justification, optimization, and dose-aware protocols form a practical safety framework.
What this means for you: imaging is ordered only when it can change your care, and the scan is tailored to your anatomy and the clinical task. If you have questions about cbct scan safety, ask about the field size, the protocol selected, and how the result will affect treatment. Clear answers should make the tradeoffs easy to understand. The right image, at the right time, keeps care safe.
Comparing CBCT to Traditional X-Rays
CBCT creates a 3D picture of your teeth and jaws, while traditional dental x-rays make a flat 2D image. The 3D view can reveal depth, angles, and hidden structures that a single film cannot show. For routine checks, 2D images are usually enough and use less radiation. Short scenario: planning an implant close to a nerve.
Because CBCT gathers a volume, your dentist can look at thin slices from any direction and measure exact distances. This helps find the true path of roots, the shape of bone, and the position of nerves or sinuses, which supports safer surgery and precise implant planning. In selected cases, CBCT has shown higher accuracy for finding periapical lesions compared with 2D methods, which can guide decisions about treatment or follow-up [4]. CBCT is also helpful when teeth are impacted, canals are unusual, or fractures are suspected. For example, a focused scan may help confirm implant positions when planning stable snap-in implant dentures.
Traditional x-rays remain the first choice for routine cavities, checkups, and quick problem-solving because they are fast, comfortable, and low dose. CBCT is reserved for questions that truly need 3D information, such as mapping a nerve before surgery or assessing complex infections. Effective dose with CBCT is generally higher than a bitewing or panoramic image, and lower than a conventional medical CT when imaging the jaws, so justification and tailored settings are important [5]. In practice, your dentist selects the smallest field and the right exposure to answer the question while limiting dose.
What does this mean for you? Most visits rely on simple 2D films. When your case needs more detail, a focused CBCT can clarify the picture, support cbct scan safety decisions, and reduce surprises during treatment. The key is choosing the right image for the job. The right image leads to clearer, safer care.
Safety Protocols for CBCT Scans
CBCT safety starts with justification, then careful setup to limit exposure while answering one clinical question. We apply the ALARA principle, selecting the smallest scan size that meets the need and tailoring settings to the patient. Short scenario: before an implant, a focused scan maps the site without imaging the entire jaw. These steps support cbct scan safety without sacrificing diagnostic value.
Before any scan, we confirm medical history, pregnancy status, and whether recent images already exist. If prior scans answer the question, we avoid new exposure and request those files. Trained staff use positioning lasers, head supports, and a bite tab to steady the head, which prevents blur and repeat scans. A preview and checklist confirm the region of interest, and exposure parameters are chosen for the task and patient size. Jewelry, removable appliances, and glasses are taken off, and artifact-reduction protocols are used when metal restorations are present.
We also limit which tissues are included. The field is centered on the problem area, and sensitive regions are kept outside the beam when feasible. Shielding is used only when it does not block the anatomy we must see. For children, we use child-sized fields and pediatric exposure protocols, and we scan only when the result could change care. For those who are or may be pregnant, we consider alternatives or deferral unless imaging is essential for urgent treatment.
Quality assurance supports these daily habits. The unit is calibrated on a schedule, software is updated, and staff complete ongoing training. We document dose indices and indications, and we share images securely with your specialists to avoid duplicate scans. What this means for you: the scan is planned to answer a single question with the least exposure practical. Ask which decision depends on the image and how the field was limited. One well-planned scan is safer than several repeats.
Benefits of Using CBCT in Dentistry
CBCT gives a clear 3D view of teeth, bone, nerves, and sinuses so care can be planned with precision. It helps dentists spot hidden problems, choose safer paths for treatment, and measure distances accurately. Short scenario: locating an impacted canine that does not appear clearly on 2D x-rays. The result is fewer surprises and more predictable procedures.
Three-dimensional data changes planning from guesswork to measurement. With CBCT, clinicians can gauge bone height and width, check the angle and depth for an implant, and see how close a root or planned surgery is to vital structures. This level of detail supports decisions like orthodontic traction or exposure of impacted canines by showing the exact position, orientation, and nearby risks, which improves planning and communication with patients [6]. Clear images also help teams decide when to modify a plan before treatment begins.
Endodontic care benefits as well. CBCT can reveal extra canals, root curvatures, and fractures that are not obvious on 2D films, and it is widely used to plan endodontic microsurgery by mapping critical anatomy around the tooth apex [7]. In surgery, knowing the shape of bone and the course of nerves reduces the need for exploratory steps, which can shorten chair time and limit tissue trauma. These benefits align with cbct scan safety when scans are justified, focused on the problem area, and set to the lowest exposure that still answers the clinical question.
For patients, CBCT can mean clearer options, fewer appointments, and more confidence before a procedure. Images can be rotated and sliced in the exam room, making it easier to understand why a plan was chosen and what alternatives exist. If your dentist recommends CBCT, ask which decision the scan will guide and how the field will be limited. The right 3D image, used at the right time, supports safer care.
Patient Considerations Before a CBCT Scan
Before a CBCT scan, share your medical history, any chance of pregnancy, and whether you have had recent dental images. Short scenario: a patient with a nose ring arrives for a scan. Remove removable metal items like earrings, tongue bars, glasses, and partial dentures so they do not blur the image. You will sit or stand still for less than a minute, and there is no injection or contrast.
Bringing prior x-rays or CT scans helps avoid repeat imaging and keeps exposure low. Your dentist will decide if a CBCT is needed to answer a specific question, then choose a small scan area focused on that problem. Staying very still prevents motion blur, which reduces the chance of a second scan. Tell the team if you have a strong gag reflex or neck or jaw pain so positioning can be adjusted for comfort.
If you wear braces or have metal fillings, the scan can still be useful, though some streaks may appear. Removing what is removable, such as retainers, aligners, and jewelry, improves clarity. For children, expect a shorter, child-sized scan with supports to help them hold still. If you are pregnant or think you might be, tell your dentist so timing and alternatives can be considered for non-urgent needs.
Share any history of surgeries, implants, sinus problems, or facial trauma, as these details guide where the scan is aimed. Anxiety is common, especially if you dislike tight spaces. Simple breathing coaching and a brief practice position usually help. For those who remain very anxious, ask about our oral sedation options, which may make it easier to stay still for clear images.
Good questions to ask include: Why is this scan needed, which area will be imaged, and how will the result change my treatment plan? Understanding the purpose, field size, and expected benefit helps you weigh cbct scan safety with clinical value. One focused, well-planned scan can prevent guesswork and improve care decisions. The right preparation leads to clearer images and smoother visits.
Interpreting CBCT Results
Interpreting CBCT results means reading the 3D scan slice by slice and as a full volume. The dentist checks image quality, reviews the anatomy from several angles, and makes precise measurements. Findings are matched with your symptoms and exam. A clear summary then explains what was seen and how it affects care.
Short scenario: a premolar hurts when chewing. First, we confirm the scan covers the right area and is free of motion blur. Brightness and contrast are adjusted so enamel, dentin, and bone are easy to see. The volume is studied in axial, coronal, and sagittal planes, then along the curve of the jaw where needed. We look for root cracks, extra canals, bone changes, the position of nerves and sinuses, and any unusual spaces or lesions. Measurements guide decisions, such as how far a site is from a nerve or sinus, or whether bone is thick enough for an implant.
Next, we connect images to your specific question. Pain patterns, cold or bite tests, and your history help confirm whether a finding explains the symptoms. Everything inside the scanned field is still reviewed, even if it is not the main concern, because CBCT can reveal unrelated findings that matter. Significant changes outside the teeth, like sinus lining thickening, are documented and may prompt referral to a radiologist or your physician. We also explain limits, including less soft tissue detail and streaks from metal, so you understand what the scan can and cannot show. This careful process supports cbct scan safety by reducing repeat scans and focusing treatment.
Finally, results are shared in simple language with images on the screen. You can see the nerve canal, the sinus floor, or a hidden canal while we outline choices and next steps. Good questions include what was found, how certain we are, and how each option manages risk and recovery. Clear interpretation turns complex 3D data into confident, safer care.
Reducing Risks During Imaging Procedures
Risk is reduced by asking a clear clinical question, then tailoring the scan to answer only that question. We keep the field small, choose patient-sized settings, and prevent motion so a single scan is enough. Short scenario: a wiggly child needs a quick, steady, focused image. These steps support cbct scan safety while preserving image quality.
Good planning happens before the scan starts. We review medical history and any recent images to avoid repeats, then select a region that covers only the area of interest. A positioning “pause” confirms the site, bite support, and head alignment. When possible, we use shorter exposure modes, pulsed beams, and settings matched to the person’s size to limit dose while keeping details clear.
Clear instructions reduce movement and artifacts. We coach you to stand or sit tall, place teeth lightly together or on a bite tab, keep the tongue still, and hold your breath for a brief moment. Removable metal items, such as earrings and partial dentures, are taken out so they do not streak the image. With braces or other fixed metal, artifact‑reduction protocols help preserve diagnostic areas. If a patient cannot hold still due to pain or limited mobility, supports are adjusted so posture is comfortable and stable.
We also limit which tissues are exposed. Sensitive regions are kept outside the beam when feasible, and shields are used only when they will not block the anatomy we must see. For children, we use child-sized fields and reduced exposure settings. During pregnancy, non-urgent imaging may be deferred, and alternatives are considered if the information can wait. A test preview helps verify alignment so we do not need a second scan.
Quality processes back up these habits. Equipment is calibrated on schedule, software is updated, and staff complete ongoing training. We document indications and dose indices, then share images securely with your other providers to prevent duplicate scans. What this means for you: a well-planned, steady, and focused scan answers the question with the least exposure practical. One accurate scan is safer than several repeats.
Frequently Asked Questions
Here are quick answers to common questions people have about CBCT in Dentistry: Safety and Benefits in Glendale, AZ.
- What is a CBCT scan used for in dentistry?
A CBCT scan in dentistry provides a 3D view of the teeth, jaw, nerves, and sinuses. It is especially useful for planning procedures like implants or assessing complex cases such as impacted teeth. Unlike traditional X-rays, CBCT allows dentists to view thin slices from various angles, revealing hidden structures like extra tooth canals, bone details, or the location of nerves. This comprehensive view helps in mapping treatments, minimizing risks during procedures, and guiding precise surgeries.
- Is a CBCT scan safe, and how is exposure managed?
A CBCT scan involves more radiation than a typical dental X-ray but significantly less than a full medical CT scan. Dentists manage safety by using the smallest field of view necessary and adjusting settings to balance detail with dose. The use of pulsed x-ray beams and short scan times further limits exposure. For children and pregnant patients, extra precautions ensure scans are only performed when absolutely essential. These measures help keep radiation exposure as low as reasonably possible.
- How does a CBCT scan differ from standard dental X-rays?
A CBCT scan provides a 3D image of dental structures, allowing for detailed views from multiple angles. This is different from standard X-rays, which offer a 2D snapshot. The additional detail from CBCT is valuable for complex diagnostics and planning, such as placing dental implants near nerves. While traditional X-rays are sufficient for routine checks with lower radiation, CBCT is reserved for cases needing in-depth analysis.
- What should I expect during a CBCT scan?
During a CBCT scan, you will sit or stand still while the machine rotates around your head, capturing images from various angles. The scan is quick, usually taking less than a minute. You may be asked to remove jewelry, eyeglasses, or other metal objects to prevent image distortion. It is important to stay very still to avoid the need for repeat scans. If you have specific needs like a strong gag reflex, inform your dentist to ensure comfort.
- Can CBCT scans detect issues not visible on regular X-rays?
Yes, CBCT scans can reveal features missed in regular X-rays, such as detailed root structures, hidden fractures, and precise locations of nerves or blood vessels. This ability is critical in complex dental procedures, helping to plan accurate implant placements, assess the full extent of injuries, or identify conditions like cysts and tumors early. The comprehensive 3D data aids in better diagnosis and treatment planning, enhancing safety and effectiveness.
References
- [1] Effect of rotation axis and modulation on x-ray emission in dose assessment in panoramic radiographs using the Monte Carlo method. (2026) — PubMed:41916334 / DOI: 10.1088/1361-6498/ae597a
- [2] Monte Carlo calculations of the radiation absorbed dose to a fetus of a pregnant patient from a dental bitewing X-ray exposure. (2026) — PubMed:41821463 / DOI: 10.1093/rpd/ncaf174
- [3] Feasibility of Artificial Intelligence-Processed Low-Dose Cone-Beam Computed Tomography in Dental Imaging. (2026) — PubMed:41899835 / DOI: 10.3390/bioengineering13030304
- [4] Comparison of Diagnostic Accuracy of Different Radiographic Techniques in Diagnosing Periapical Lesions: A Clinical Study. (2025) — PubMed:41846789 / DOI: 10.4103/jpbs.jpbs_429_25
- [5] Digital Dental Radiology and Diagnostics-From 2D to 3D. (2025) — PubMed:41277722 / DOI: 10.1111/adj.70024
- [6] Diagnostic, predictive, and therapeutic approaches for impacted canines: a systematic review and meta-analysis. (2026) — PubMed:41807950 / DOI: 10.1186/s12903-026-08072-5
- [7] Advances and clinical benefits of endodontic microsurgery: A contemporary perspective. (2026) — PubMed:41982184 / DOI: 10.1002/cap.70025